FDA Panel Backs Vaccinating Pregnant Mothers to Prevent RSV in Infants
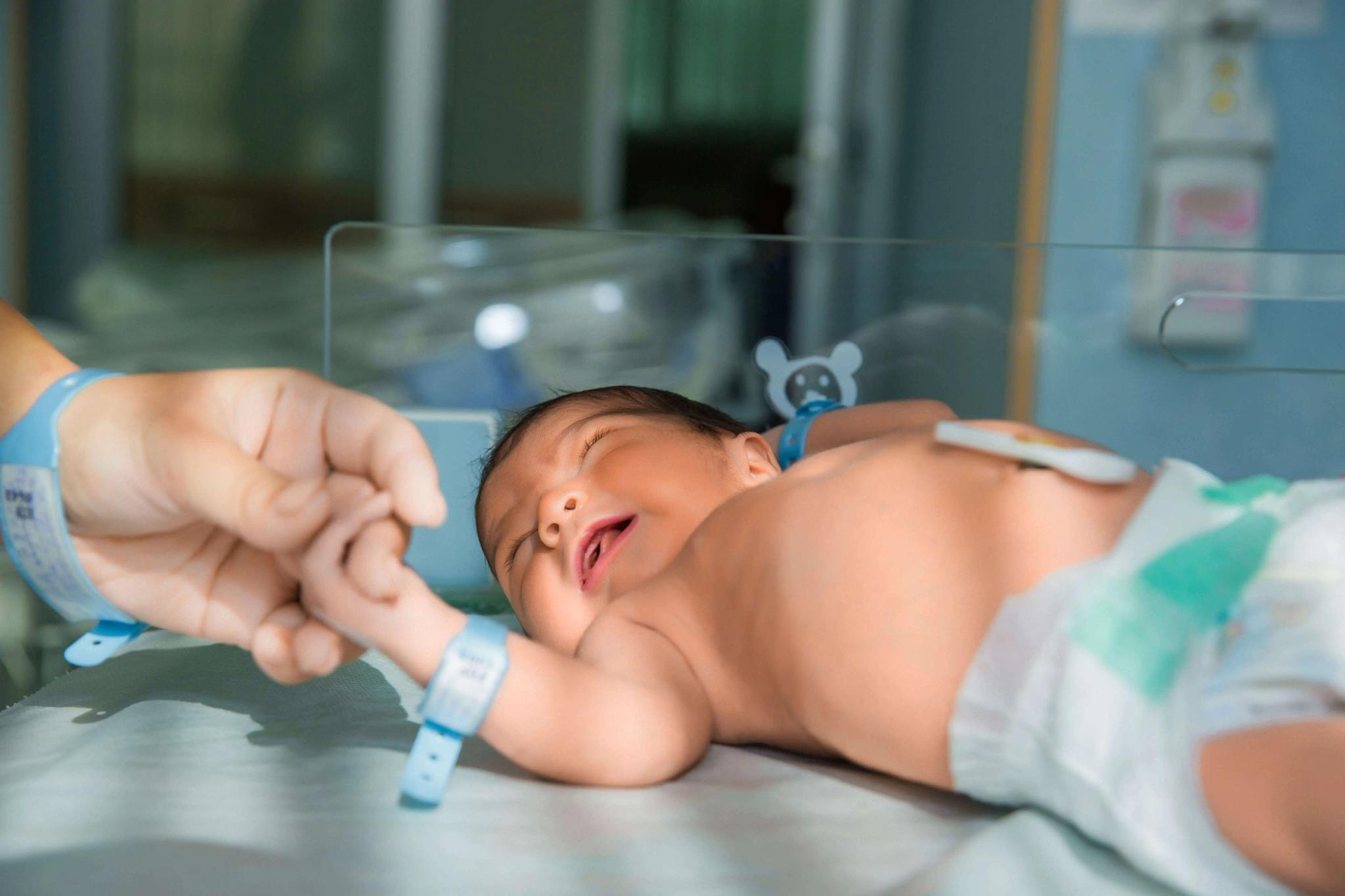
A committee of independent advisory to the Food and Drug Administration voted Thursday to recommend a vaccine that protects infants against RSV by vaccination of their mothers during pregnancy.
The 14-member panel unanimously recommended the shot, manufactured by Pfizer in the name of its effectiveness. The panel voted 10-4 to endorse it based on its safety.
If the shot gets accepted by the FDA, it will be the first vaccination that protects against respiratory syncytial disease in infants.
Also Read, The Top 3 Health Trends to Watch in 2023
"Before this pandemic began, RSV was the no. one reason for hospitalizations of infants across the United States, so this is significant," said Dr. Ofer Levy, who is the Director of the Precision Vaccines Program at Boston Children's Hospital. Levy is a non-voting part of the FDA panel but was not involved in the vote on Thursday.
Healthy adults can experience the lower respiratory illnesses that are caused by RSV is usually mild, however, it may be more severe for infants and elderly adults. The virus can kill around 300 kids less than five each annually in the U.S. and up to 10,000 people aged 65 or over according to the Centers for Disease Control and Prevention. Severe infections can lead to bronchiolitis or pneumonia causing inflammation of the airways and blocking them with mucus.
It could take a while for the FDA to decide if they want to allow the shot, but the FDA is likely to adhere to the advisory committee's recommendations.
It was announced that the FDA accepted the initial RSV vaccination this month. The vaccine was developed by the pharmaceutical giant GSK however, this shot is for people who are 60 or older.
Pfizer also offers an RSV shot to older adults awaiting FDA approval later this month. An FDA advisory group in February recommended the shot to people who are 60 or older. The same vaccine is given to women who are pregnant.
To safeguard infants, the shot is given to pregnant women from 24 to 36 weeks gestation. the antibodies that protect you are transferred into the placenta.
The members of the committee generally applauded the effectiveness of the vaccine but had reservations regarding the duration of protection as well as the possible possibility of preterm birth.
In a clinical study with more than 7,400 participants, the vaccine reduced the risk of contracting severe disease from RSV for infants by 82% approximately three months after birth. At six months, the effectiveness was about 69 percent. Children six months or younger are particularly susceptible to serious forms of RSV.
The shot also reduced the chance of developing respiratory illness caused by RSV which necessitated doctor's appointments by 51% in approximately six months. Following that the shot didn't seem to make any difference.
In a report that was released, the FDA stated that the safety data from the trial appeared "generally favorable." The most frequently reported side effects from the shot that were reported among pregnant women included headaches, fatigue muscle pain, and injection site discomfort.
However, the agency pointed out the existence of a greater number of preterm births which is defined as births occurring before 37 weeks gestation -- among those who were vaccinated (5.7%) against those who received a placebo (4.7%). The difference was not statistically significant, it's not clear if the reason was due to vaccination.
Both rates were less than what is the prevalence of premature births within the population, which is about 10 percent, according to the CDC.
In the year 2000, the pharmaceutical giant GSK stopped its study of the RSV vaccine specifically for babies because it found an increased rate of preterm birth in certain vaccine recipients.
Dr. Paul Offit, the director of the Children's Hospital of Philadelphia's Vaccine Education Centre and a representative on the FDA advisory committee, asserted that the findings of the GSK trial applied to the Pfizer study because the two vaccines have similarities.
Offit said at the hearing on Thursday, "I fear that if premature births are in any way a consequence of this vaccine, it would be unfortunate in many respects. Offit dissented from the vaccine because of its safety.
Pfizer stated that if the vaccine is accepted, the company will continue to examine the risk of premature birth among those who have received the vaccine.
Levy said that researchers typically take note of the risk of premature birth in vaccines administered to women who are pregnant.
"There is always the nagging concern: Are you contributing to any inflammation that could be dangerous? Because the body interprets inflammation as "let's get the baby out, the woman is no longer safe," Therefore, you need a relatively bland vaccine, he said.
However, Adam Berger, a researcher at the National Institutes of Health approved the vaccine based on effectiveness and safety The vaccine is urgently required.
There is no other option for prevention in this situation, and it could save a lot of lives, according to Berger.
Eleven RSV vaccines (including GSK's approved shot) are currently being studied within U.S. trials, according to information that was provided by NBC News by PATH, an international health nonprofit. Six of them are for older people and five are intended to protect infants and children.
A monoclonal antibody injection that is administered directly to infants and works similarly to a vaccine is already recognized by the FDA in Canada, Europe, and the United Kingdom. The FDA started reviewing the data on the shot in January and is scheduled to decide in the season or in the fall if it will allow the shot or not.
Business News
Pop-ups in Market East Bring Energy to Philadelphia's Languished Retail Corridor
Community-Inspired Flavors' Celebration Forest Independent Business's First Anniversary
Tariffs and Global Conflicts Squeeze California's Small Businesses
Trump, Angling War and For Violation, Invisibly Turns Back on Pakistan and Iran
What Kind of Business Model Would Help Colorado's Creative Industries?